Anatomy of a long-term care rate increase
In recent years, many carriers of long-term care insurance (LTCI) products have found themselves with high loss ratios and low profitability. The low interest rate environment, low lapse rates, and higher morbidity have contributed to these factors. Legacy LTC products have level premiums from issue that do not pay claims until many years down the road. Insurers must collect enough premium now to fund those claims later. As their LTCI blocks of business continue to deteriorate, it has become apparent to many insurers that premiums collected will not be sufficient to cover future claims and expenses. The U.S. Department of the Treasury took note of the volatile state of the LTCI industry, publishing a report last year on recommendations for improving regulation in the industry.1
One approach to remedying the challenges insurers are facing is to request approval for a rate increase. This process can be arduous and time-consuming but with the right tools and strategy, carriers can maximize their chances for approval success while minimizing strain on resources. This paper provides guidance for insurers on how to prepare clean, efficient rate increase filings and to help carriers work with regulators to incorporate the information they seek.
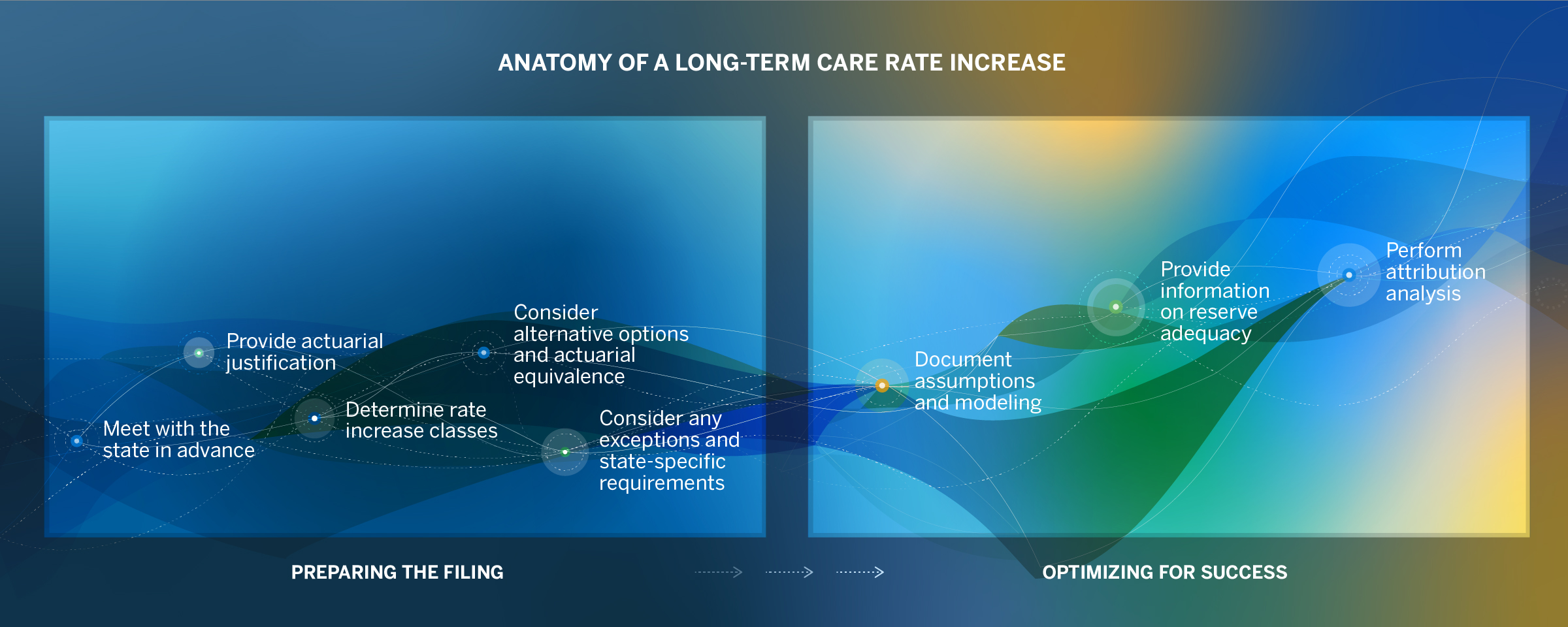
Although the LTC rate submission and approval processes vary by state, there are common elements that exist in most or all jurisdictions. This brief is organized around a common process, which is illustrated in Figure 1.
Figure 1 : Long-Term Care Rate Increase Flowchart
Preparing the filing
Meet with the state in advance. In many cases, state departments of insurance prescribe specific forms and maintain specific requirements for rate filing submissions. Carriers that meet with the state at the start of the process are demonstrating their willingness to work together with the regulator. Most regulators prefer files to be submitted in a certain format to facilitate efficiency and allow for a consistent review across different companies. They may be open to carriers providing alternative documents and/or formats—which carriers may suggest to reduce administrative burden—so long as they cover the same general information. By understanding the intention behind the information state regulators request, carriers are better able to tailor their rate requests to a state’s particular needs. The best way to come to this understanding is by meeting with the regulators and starting to build a working relationship.
Meeting with the state before starting the filing process may also help alleviate the additional work involved if regulators follow up with objections to the filings. The initial meeting can eliminate the need for future objections because the regulator may request this pertinent information up-front. This may occur when carriers disclose information that triggers the regulator to make additional requests for the initial filing. The initial meeting can also help once an objection has been generated because the carrier has already established some familiarity with the regulator reviewing the filing.
Provide actuarial justification. Actuarial justifications (e.g., pre- and post-rate stabilization, loss ratio approach, if-knew2) must comply with the regulation of the state. In some cases, however, the insurance commissioner and reviewers may apply their judgment in assessing rate requests beyond the minimum standards specified in the regulations. Different approaches for actuarial justification have been summarized in the document, “Approaches to Reviewing Premium Rate Increases” published by the NAIC Long-Term Care (LTC) Pricing Subgroup.3 One of the considerations of the various approaches is not allowing insurance companies to recoup past losses, which is defined and discussed in the paper. The publication describes the following approaches:
- Lifetime loss ratio
- Prospective present value
- Blended if-knew makeup approach
- 2014 NAIC model regulation
All of these approaches include several different calculations and definitions. The publication also provides definitions on how the policy is treated as it transitioned through various policy statuses during the past life of the policy (e.g., premium paying to paid up) and shows sample calculations. The examples we discuss later refer to if-knew (a component of the blended if-knew makeup approach) and the lifetime loss ratio approach.
Because the state departments of insurance may have approved different levels of rate increases historically, the current rates for a given LTC policy may differ from state to state. Under the lifetime loss ratio approach, if, for example, a carrier is filing in State A but has experience in both states, the carrier may choose to reprice the State B experience to a State A rate basis, or choose to leave State B experience as is. Depending on the credibility of a particular state in which the carrier is requesting a rate increase, the carrier may be able to show just the experience for that state.
In addition, regulators may request the lifetime loss ratio with the current rate basis all the way back to inception (“since inception”). Restating past premium to assume the proposed rate increase from inception is a potentially controversial actuarial approach to assessing a block of LTC as the carrier did not actually collect that level of premium and the results produce artificial loss ratios. While states often try to prevent situations where the carrier is recouping past losses, this approach does not consistently achieve that goal and should be evaluated on a case-by-case basis.
Note that the American Academy of Actuaries also provides guidance on this topic.4
Determine rate increase classes. When considering the actuarial justification for a rate increase, the actuary and management often find it beneficial to segment the block of business by certain policy parameters; in fact, some state regulators may even prescribe specific rate increase class segmentation. The analysis may indicate that certain policy classes need higher rate increases than other policy classes. For example, policies with short benefit periods may have very different historical and projected cash flow patterns than policies with longer benefit periods. If appropriate, carriers may consider requesting different rate increases for each segment, or rate increase class.
Looking at a policy's if-knew premium (i.e., the premium a carrier would have charged at issue assuming pricing assumptions developed today were used in premium development back then) may help to inform potential correlation in variables or policy language that are contributing to poor experience. For the sake of getting a seriatim result, the actuary could use the current best estimate assumptions from cash flow testing and calculate the net premium and divide the result by 60% to calculate a net level if-knew premium. The actuary may also want to consider early duration fit of assumptions to historical experience (this is relevant to the lifetime loss ratio calculation even if it may not be relevant for cash flow testing and modeling the business going forward). Comparing this to the current baseline could help understand whether inflation, elimination period, or other policy features are the best class segmentation even if they are not the ultimate actuarial justification used.
Although looking at the LTC block by certain policy buckets may uncover meaningful differences, certain rate increase classes may not be credible. For example, if, after examining emerging experience, a carrier is considering bucketing policies into rate increase classes based on inflation type but has very few policies with one particular inflation type, then the carrier may consider bucketing this class with another class deemed similar. This can be accomplished by finding another policy characteristic on which to base the classes that still presents the deterioration of business. Alternatively, a carrier may consider not requesting a rate increase on the few policies with an infrequent policy inflation feature in order to present a strong case for the policies in other inflation classes.
Note that there is no common standard for credibility in long-term care insurance. Many factors go into the consideration of credibility, including amount of exposure, mix of risks, trends over time, and consistency of results. No single, rigid formula (or credibility value) is used. Typically, as a guide, actuaries assume that 1,082 claims would be fully credible. This number was determined based on the Longley-Cook credibility table as the number of claims that gives 90% confidence that the true actual-to-expected (A/E) level is within 5%. Other credibility measures are possible and would produce different results.
Consider alternative options and actuarial equivalence. Reviewing the rate increase classes and the variables that are leading to deteriorating experience may inform the alternative options that the company may wish to offer. Landing spots and inflation downgrades are popular. By regulation, the company must always offer a nonforfeiture option.
Alternative options are usually offered so that insureds can choose the approach that best fits their specific situations. In some situations, an insured’s inflation benefit may have resulted in currently being over-insured for that person's LTC risk and therefore the benefit reduction coupled with a premium reduction may be the best option. For some individuals, the impact will be larger for the rate increase, and for others the actuarial impact will be larger for the downgrade.
There are many different considerations when offering a reduced benefit option, such as the type of benefit to offer and the definition of actuarial equivalence. These options are discussed further in a recent Milliman whitepaper5 and Society of Actuaries publication.6
Consider any exceptions and state-specific requirements. Several states have specific requirements that a carrier must comply with in order to submit a filing. Always check the state’s website and the System for Electronic Rates and Forms Filing (SERFF) for readily available information, such as forms and documents, to better prepare for the initial meeting with the state regulator.
Optimizing for success
While regulators in different states may have specific requests, there are several ways issuers can optimize their filings to accommodate most regulators’ needs. Specifically, the actuary may want or need to attach one or more of the following analyses or exhibits below to a filing to increase their chance for approval success.
Document assumptions and modeling. Regulators often seek to gain more insight on how insured lives, premiums, and claim projections are modeled. Specifically, regulators want to understand how the various morbidity (i.e., assumptions related to the probability of going on claim and staying on claim), demographic, and economic assumptions are combined to produce the actuarial justification. Along these lines, regulators may also want to ensure the assumptions used in modeling are appropriate. They may request actual-to-expected analyses and qualitative descriptions of assumption development to see how assumptions have evolved over time. For example, an actual-to-expected analysis on lapse (i.e., the probability that a policyholder stops paying premiums or voluntarily terminates coverage), would compare the assumed lapse rates in modeling to the company’s actual lapse experience over a recent time period and calculate the percentage difference between the two. Actual-to-expected analyses on mortality and morbidity assumptions for original assumptions, prior rate increase assumptions, and current assumptions are also commonly requested.
Provide information on reserve adequacy, surplus, and state subsidization. Reserves may be scrutinized as part of a rate increase request. Long-term care reserves are funds that a carrier sets aside to cover claim payments that are expected to occur in the future. Companies must estimate their reserves using one of several available techniques, most of which involve analyzing prior claim data. Regulators may seek assurance that a company does not have too much margin, which may be used to justify a larger rate increase than necessary. To this end, carriers can provide retrospective tests on claim liabilities, illustrating the amount of sufficiency or deficiency in the claim reserves. Retrospective tests sum a prior period’s paid claims plus estimated reserves and compare them to the actual incurred claims. A close match validates that the reserving methodology used properly approximates incurred claims.
In addition, regulators may request projected income statements, gross premium valuation (GPV) calculations, and prior financial statements to understand the company’s current financial solvency situation and how that impacts the company’s ultimate need for a rate increase. The regulators may be interested in what level of rate increase has been granted already in various states, most commonly their own, and also nationwide.
Perform attribution analysis. In the early years of offering private long-term care insurance, many carriers significantly underpriced policies. Underpricing occurred because long-term care products were still relatively new, there was limited actuarial data, and there was inherent uncertainty around predicting payments far into the future. As carriers have monitored their blocks of business over the last few decades, they have revised their assumptions to be more appropriate based on emerging experience, resulting in far less favorable projections. An attribution analysis quantifies how each assumption contributed to the change in loss ratio. Creating an attribution analysis involves calculating premium, claims, and lifetime loss ratio projections using original pricing assumptions (and/or prior rate filing assumptions) and using current pricing assumptions. Carriers may also calculate several intermediate “steps” in which one assumption is updated at a time from original to current. Attribution analysis can be helpful to regulators because it illustrates clearly what assumptions were misestimated at pricing, causing experience to deteriorate to such a degree it necessitates a premium increase.
Figures 2 and 3 each show a sample attribution analysis using the lifetime loss ratio calculation for a two-year benefit period product and a lifetime benefit period product, respectively. As shown, the lifetime loss ratio for a two-year benefit period is significantly better, which may make it appropriate to have these two different benefit periods in separate rate increase classes (as discussed earlier). We also calculate the needed cumulative future rate increase using a lifetime loss ratio approach and a since-inception approach.
Figure 2 is an illustrative example of the impact to the loss ratio of revising to current assumptions. Note that this figure illustrates a two-year benefit period, zero-day elimination period policy priced at a 60% loss ratio with no inflation protection and priced in 1992.
Figure 2: Impact to Loss Ratio of Revising Assumptions, Two-Year Benefit Period
- 8% discount rate revised to a 4% discount rate
- 1980 CSO mortality revised to 2012 IAM mortality
- Ultimate rate of 6% lapse revised to an ultimate rate of 1% lapse
- 1992 morbidity base revised to a 2017 morbidity base
- Cumulative rate increase of 300% between 1992 and 2020
- No additional future rate increases are needed to meet 85%7 loss ratio
Similarly, Figure 3 also illustrates the impact to the loss ratio of revising to current assumptions, with zero-day elimination period policy priced at a 60% loss ratio, no inflation protection, and priced in 1992. But this figure illustrates a lifetime benefit period.
Figure 3: Impact to Loss Ratio of Revising Assumptions, Lifetime Benefit Period
- 8% discount rate changed to a 4% discount rate
- 1980 CSO mortality revised to 2012 IAM mortality
- Ultimate rate of 6% lapse revised to an ultimate of 1% lapse
- 1992 morbidity base revised to a 2017 morbidity base
- Cumulative rate increase of 260% between 1992 and 2020
- Cumulative rate increase of 200% needed after 2020 to meet 85% loss ratio; alternatively, no rate increase would be needed had the historical cumulative rate increase of 300% been applied since inception
These figures illustrate the drivers of a rate increase. It is important to recognize the need for a rate increase before the block of business becomes too small to ever achieve the rate increase needed for sustainability.
Summary
This paper serves as a basic reference guide and a simple walkthrough of the rate increase filing process for LTCI carriers. Stakeholders, carriers, and regulators want to ensure carrier solvency and protect the health and financial well-being of policyholders within each state.
The National Association of Insurance Commissioners (NAIC) Long Term Care (EX) task force recognizes the need for “a consistent national approach for reviewing LTCI rates that results in actuarially appropriate increases being granted by the states in a timely manner and eliminates cross-state rate subsidization."8 Although the process in the future might look different from what we outlined in this paper, the actuarial issues and discussions will still be relevant as the process evolves.
1U.S. Department of the Treasury (August 2020). Long-Term Care Insurance: Recommendations for Improvement of Regulation. Retrieved January 6, 2021, from Report-Federal-Interagency-Task-Force-Long-Term-Care-Insurance.pdf (treasury.gov).
2“If-knew increase—increase to the premium rates such that the resulting rates, if in effect from inception of the form, would produce the greater of the initial target lifetime loss ratio or minimum loss ratio applicable to the form.” NAIC LTC Pricing subgroup. (October 2018). Long-term Care Insurance: Approaches to Reviewing Premium Rate Increases. Retrieved January 20, 2021, from https://content.naic.org/sites/default/files/inline-files/committees_b_ltca_wg_approaches_ltc_rate_increases_final.docx (Word download). .
3NAIC LTC Pricing Subgroup (October 2018). Long-term Care Insurance: Approaches to Reviewing Premium Rate Increases. Retrieved January 6, 2021, from https://content.naic.org/sites/default/files/inline-files/committees_b_ltca_wg_approaches_ltc_rate_increases_final.docx (Word download).
4American Academy of Actuaries (October 2018). Long-Term Care Insurance: Considerations for Treatment of Past Losses in Rate Increase Requests. Retrieved January 6, 2021, from https://www.actuary.org/content/long-term-care-insurance-considerations-treatment-past-losses-rate-increase-requests.
5Eaton, R. (April 2020). Developing Alternative Options During LTC Premium Rate Increases. Society of Actuaries Long-Term Care News. Retrieved January 6, 2021, from https://www.milliman.com/en/insight/developing-alternative-options-during-ltc-premium-rate-increases-company.
6Bergerson, M. & Hebig, J. (April 2017). Detail Matters: Level vs. Relative Premium Increases and Their Effect on Actuarial Equivalence in Long-Term Care Insurance. Society of Actuaries Long-Term Care News, p. 29. Retrieved January 6, 2021, from https://www.soa.org/globalassets/assets/library/newsletters/long-term-care/2017/april/ltc-2017-iss44.pdf.
7NAIC (Q1 2017). Long-Term Care Insurance Model Regulation, p. 28. Retrieved January 6, 2021, from https://content.naic.org/sites/default/files/inline-files/MDL-641.pdf.
8NAIC. Long-Term Care Insurance (EX) Task Force. Retrieved January 6, 2021, from https://content.naic.org/cmte_ex_ltci_tf.htm
Explore more tags from this article
About the Author(s)
Rachel Marsiglio
Chicago Tel: Tel +1 312 726 0677 | Fax +1 312 499 5685 | Direct +1 312 577 2887
View bioContact us
We’re here to help you break through complex challenges and achieve next-level success.